- Products
 SpiroScout®
SpiroScout® Spirometer system
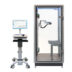 PowerCube™ Body+
PowerCube™ Body+ Plethysmograph
 PowerCube™ Spiro+
PowerCube™ Spiro+ Enhanced PFT Station
 PowerCube™ Diffusion+
PowerCube™ Diffusion+ Diffusion workstation
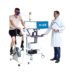 PowerCube™ Ergo
PowerCube™ Ergo CPET
 Provo.X
Provo.X Provocation system
 EucapSys
EucapSysEVH provocation
 AltiTrainer
AltiTrainerAltitude simulation
 tremoflo
tremofloOscillometry
 EDAN i20
EDAN i20 Blood gas & chemistry
 Vivatmo pro
Vivatmo proFeNO monitoring
 SpiroDef
SpiroDefPFT filter series
- Software
- Company
- Support
The art of lung diagnostics.
Quick Access
Pulmonary function 3 months after hospitalization for COVID-19
Reliable, safe and easy-to-use filter for pulmonary function diagnostics.
The long-term pulmonary consequences of coronavirus disease are not yet known. The aim of a recently published ERS study was to describe self-reported dyspnea, quality of life, pulmonary function, and chest computed tomography results 3 months after hospitalization for COVID-19. The investigators anticipated that the data and descriptions would be worse in patients admitted to intensive care units than in the comparison group. For this purpose, 103 COVID-19 patients were enrolled in a cohort study after their hospital discharge from several Norwegian hospitals. Among them were 15 patients who had been treated in intensive care units.

The mMRC score was > 0 in 54% and > 1 in 19% of participants. Median (25th-75th percentile) forced vital capacity and forced expiratory volume in 1 s were 94% (76-121%) and 92% (84-106%) of prediction, respectively. DLCO was just under a quarter below the lower limit of normal. Ground glass opacities (GGO) with a distribution greater than 10% in at least one of the four lung zones were present in 25% of participants, while 19% had parenchymal bands on chest CT.
ICU survivors had similar dyspnea scores and lung function to non-ICU patients, but a higher prevalence of GGO (adjusted OR 4.2, 95% CI 1.1-15.6) and lower performance of simple activities.
At 12 weeks after hospitalization for COVID-19, a quarter of participants had chest opacities and decreased diffusion capacity on CT. Intensive care unit admission was associated with pathologic CT findings. This was not reflected in increased dyspnea or impaired pulmonary function.